BUPRENORPHINE STADA 70 micrograms/hour transdermal patch 96 hours

How to use BUPRENORPHINE STADA 70 micrograms/hour transdermal patch 96 hours
Translated with AI
This page provides general information and does not replace a doctor’s consultation. Always consult a doctor before taking any medication. Seek urgent medical care if symptoms are severe.
Show originalContents of the leaflet
Introduction
Leaflet: information for the user
Buprenorphine Stada 35 micrograms/hour transdermal patch 96 hours EFG
Buprenorphine Stada 52.5 micrograms/hour transdermal patch 96 hours EFG
Buprenorphine Stada 70 micrograms/hour transdermal patch 96 hours EFG
Read the entire leaflet carefully before starting to use this medicine, as it contains important information for you.
- Keep this leaflet, as you may need to read it again.
- If you have any questions, ask your doctor or pharmacist.
- This medicine has been prescribed to you only, and you should not give it to others, even if they have the same symptoms as you, as it may harm them.
- If you experience side effects, consult your doctor or pharmacist, even if they are not listed in this leaflet. See section 4.
Contents of the leaflet
- What is Buprenorphine Stada and what is it used for
- What you need to know before taking Buprenorphine Stada
- How to use Buprenorphine Stada
- Possible side effects
- Storage of Buprenorphine Stada
- Contents of the pack and further information
1. What is Buprenorphine Stada and what is it used for
The active substance of Buprenorphine Stada is buprenorphine.
Buprenorphine is an analgesic (a pain-relieving medicine) indicated for the relief of moderate to severe cancer pain and severe pain that does not respond to other types of analgesics. Buprenorphine acts through the skin. Buprenorphine is an opioid (a strong pain-relieving medicine) that reduces pain by acting on the central nervous system (in specific nerve cells in the spinal cord and brain). The effect of the transdermal patch lasts up to a maximum of four days. Buprenorphine is not suitable for the treatment of acute (short-term) pain.
2. What you need to know before taking Buprenorphine Stada
Do not use Buprenorphine Stada
- if you are allergic to buprenorphine or any of the other ingredients of this medicine (listed in section 6);
- if you are addicted to strong painkillers (opioids);
- if you have a disease that makes it difficult for you to breathe or may cause breathing difficulties;
- if you are taking MAO inhibitors (certain medicines for the treatment of depression) or have taken them in the last two weeks (see "Using Buprenorphine Stada with other medicines");
- in case of myasthenia gravis (a type of severe muscle weakness);
- in case of delirium tremens (confusion and tremors caused by alcohol withdrawal after habitual excessive alcohol consumption or during a period of high alcohol consumption);
- in case of pregnancy.
Buprenorphine should not be used to treat withdrawal syndrome in drug addicts.
Warnings and precautions
Consult your doctor or pharmacist before starting to use Buprenorphine Stada
- if you have recently consumed a lot of alcohol,
- if you have epileptic seizures or convulsions (fits),
- if you have altered consciousness (feeling dizzy or faint) for unknown reasons,
- if you are in shock (a sign could be cold sweat),
- if you have increased intracranial pressure (e.g., after head injury or brain disease) without the possibility of artificial respiration,
- if you have difficulty breathing or are taking other medication that may cause you to breathe more slowly or weakly (see "Using Buprenorphine Stada with other medicines"),
- if you have liver problems,
- if you have a tendency to abuse medicines or drugs.
- if you have depression or other diseases that are treated with antidepressants.
The use of these medicines together with buprenorphine may cause serotonin syndrome, a potentially life-threatening disease (see "Using Buprenorphine Stada with other medicines").
Also, note the following precautions:
? Some people may become dependent on strong painkillers such as buprenorphine when they use them for a long time. These patients may experience effects after they stop using them (see "If you stop taking Buprenorphine Stada").
? Fever and heat can lead to higher-than-normal amounts of buprenorphine in the blood. Also, heat can prevent the transdermal patch from sticking properly. Therefore, consult your doctor if you have a fever and avoid exposure to heat sources (e.g., sauna, infrared lamps, electric blankets, or hot water bottles).
Athletes should be warned that this medicine may give a positive result in doping tests.
Children and adolescents
Buprenorphine should not be used in people under 18 years of age, as there is no experience with this age group to date.
Sleep-related breathing disorders
Buprenorphine may cause sleep-related breathing disorders such as sleep apnea (pauses in breathing during sleep) and sleep-related hypoxemia (low oxygen levels in the blood). Symptoms may include pauses in breathing during sleep, nighttime awakenings due to difficulty breathing, difficulty maintaining sleep, or excessive daytime sleepiness. Contact your doctor if you or someone else observes these symptoms. Your doctor may consider a dose reduction.
Tolerance, dependence, and addiction
This medicine contains buprenorphine, which is an opioid medicine. Repeated use of opioids can make the medicine less effective (the body gets used to it, which is known as pharmacological tolerance). Repeated use of buprenorphine can also lead to dependence, abuse, and addiction, which can result in a potentially life-threatening overdose. The risk of these side effects may be higher with a higher dose and longer use.
Dependence or addiction can cause a feeling of lack of control over the amount of medicine you need to use or how often you need to use it.
The risk of dependence or addiction varies from person to person. The risk of becoming dependent on or addicted to buprenorphine may be higher if:
- You or any member of your family have abused alcohol or experienced dependence on it, prescription medicines, or illegal drugs ("addiction").
- You are a smoker.
- You have had problems with your mood (depression, anxiety, or personality disorder) or have been treated by a psychiatrist for other mental illnesses.
If you notice any of the following symptoms while using buprenorphine, it could be a sign of dependence or addiction:
- You need to use the medicine for longer than prescribed by your doctor.
- You need to use a higher dose than recommended.
- You use the medicine even when it does not help relieve pain.
- You use the medicine for reasons other than those prescribed, for example, "to feel calm" or "to help you sleep".
- You have made repeated unsuccessful attempts to stop using the medicine or control its use.
- You feel unwell when you stop using the medicine, and you feel better once you take it again ("withdrawal effects").
If you notice any of these signs, consult your doctor to determine the best treatment option for you, when it is appropriate to stop the medicine, and how to do it safely (see section 3, if you stop taking Buprenorphine Stada).
Other medicines and Buprenorphine Stada
Tell your doctor or pharmacist if you are using, have recently used, or might use any other medicines.
Some medicines may increase the side effects of buprenorphine and may occasionally cause very serious reactions. Do not take any other medicine while taking buprenorphine without consulting your doctor first, especially:
? Antidepressants such as moclobemide, tranilcipromine, citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, sertraline, duloxetine, venlafaxine, amitriptyline, doxepin, or trimipramine. These medicines may interact with buprenorphine, and you may experience symptoms such as involuntary muscle contractions, including muscles that control eye movement, agitation, hallucinations, coma, excessive sweating, tremors, exaggerated reflexes, increased muscle tension, and body temperature above 38 °C. Contact your doctor if you experience these symptoms.
? Buprenorphine should not be used with MAO inhibitors (certain medicines for the treatment of depression) or if you have taken them in the last two weeks.
? Buprenorphine may cause some patients to feel drowsy, vomit, feel dizzy, or breathe more slowly or weakly. These side effects may be intensified if you take other medicines that may cause the same effects. These other medicines include other strong painkillers (opioids), certain sleep aids, anesthetics, and medicines for the treatment of certain psychological disorders (tranquilizers, antidepressants, and antipsychotics).
- The concomitant use of buprenorphine with sedative medicines such as benzodiazepines or related medicines increases the risk of sedation, respiratory depression, coma, or even death. Due to this, concomitant use should only be considered when other treatment options are not possible. However, if your doctor prescribes buprenorphine with sedatives, the dose and duration of concomitant treatment should be limited by your doctor.
Inform your doctor about all sedative medicines you are taking and closely follow your doctor's dosing recommendations. It may be helpful to inform friends or relatives so they are aware of the signs and symptoms indicated above. Contact your doctor when you experience these symptoms.
- If buprenorphine is used with some medicines, the effect of the transdermal patch may be intensified. These medicines include, for example, certain anti-infectives and antifungals (e.g., those containing erythromycin or ketoconazole) or medicines for HIV (e.g., those containing ritonavir).
- If buprenorphine is used with other medicines, the effect of the transdermal patch may be reduced. These medicines include, for example, dexamethasone, certain products for the treatment of epilepsy (e.g., those containing carbamazepine or phenytoin) or medicines used for the treatment of tuberculosis (e.g., rifampicin).
- Gabapentin or pregabalin for treating epilepsy or pain due to nerve problems (neuropathic pain)
- Medicines for treating allergies, dizziness, or nausea (antihistamines or antiemetics)
- Medicines for treating psychiatric disorders (antipsychotics or neuroleptics)
- Muscle relaxants
- Medicines for treating Parkinson's disease
Using Buprenorphine Stada with food, drinks, and alcohol
Do not drink alcohol while using buprenorphine. Alcohol may intensify certain side effects of the transdermal patch, and you may not feel well.
Pregnancy, breastfeeding, and fertility
If you are pregnant or breastfeeding, think you may be pregnant, or plan to become pregnant, consult your doctor or pharmacist before using this medicine.
There is not enough experience with the use of buprenorphine in pregnant women to date. Therefore, buprenorphine should not be used during pregnancy.
Buprenorphine, the active ingredient in the transdermal patch, passes into breast milk and inhibits milk production. Therefore, buprenorphine should not be used during breastfeeding.
Driving and using machines
Buprenorphine may make you feel dizzy, drowsy, or have double or blurred vision and may affect your reflexes so that you do not react adequately or quickly enough in case of sudden or unexpected situations. This applies especially:
- at the start of treatment
- when changing the dose
- when switching from another medicine to buprenorphine
- if you are also taking other medicines that act on the brain
- if you drink alcohol
If you are affected, you should not drive or operate machinery while using buprenorphine. This also applies at the end of treatment with buprenorphine. Do not drive or operate machinery for at least 24 hours after removing the patch.
In case of doubt, consult your doctor or pharmacist.
3. How to use Buprenorphine Stada
Follow the administration instructions for this medication exactly as indicated by your doctor. In case of doubt, consult your doctor or pharmacist again.
Before starting treatment and on a regular basis during treatment, your doctor will also explain what you can expect from using buprenorphine, when and for how long you should use it, when you should contact your doctor, and when you should stop using it (see also "If you stop treatment with Buprenorphine Stada").
Buprenorphine Stada is available in three doses: buprenorphine 35 micrograms/hour transdermal patch 96 hours, buprenorphine 52.5 micrograms/hour transdermal patch 96 hours, and buprenorphine 70 micrograms/hour transdermal patch 96 hours.
Your doctor has chosen this buprenorphine patch as the most suitable for you.
During treatment, your doctor may change the transdermal patch you use to a smaller or larger one if necessary.
Do not cut or divide the patch.
The recommended dose is:
Adults
Follow these instructions unless your doctor has given you different instructions.
Apply buprenorphine (as detailed below) and change it after four days, at most. To facilitate use, you can change the patch twice a week on fixed days, e.g., "always on Monday morning and Thursday afternoon". To help you remember when to change the patch, note it on the packaging. If your doctor has instructed you to take other painkillers in addition to the transdermal patch, follow your doctor's instructions strictly; otherwise, you will not fully benefit from the treatment with buprenorphine.
Elderly patients
No dose adjustment is required in elderly patients.
Patients with renal impairment/patients on dialysis
In patients with renal impairment and patients on dialysis, no dose adjustment is needed.
Patients with hepatic impairment
In patients with hepatic impairment, the intensity and duration of the action of buprenorphine may be affected. If you belong to this group of patients, your doctor will monitor you more closely.
Use in children and adolescents
Buprenorphine should not be used in people under 18 years of age because there is no experience with this age group to date.
Route of administration
Apply via the transdermal route.
When the transdermal patch is applied to the skin, the active ingredient buprenorphine passes through it to reach the blood.
Method of administration
Before applying a transdermal patch
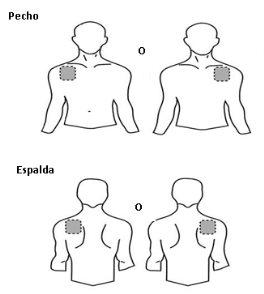
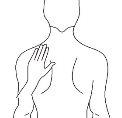
? Choose a smooth, hairless area of skin on the upper part of your body, preferably under the clavicle on the chest or on the upper back (see adjacent figure). Ask for help if you cannot apply the transdermal patch yourself. |
|
? If the chosen area has hair, cut it with a pair of scissors. Do not shave!
? Avoid areas of the skin that are red, irritated, or have any other type of spots, such as large scars.
? The area of skin you choose must be dry and clean. If necessary, wash it with cold or warm water. Do not use soap or other detergents. After a hot bath or shower, wait until your skin is completely dry and cool. Do not apply lotions, creams, or ointments to the chosen area. This could prevent the transdermal patch from sticking properly.
Applying the transdermal patch:
Step 1: Each transdermal patch is sealed in a pouch. Just before use, cut the pouch with a pair of scissors along the sealed edge. Take the transdermal patch. |
|
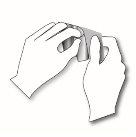
Step 2: The adhesive side of the transdermal patch is covered by a transparent protective film. Carefully peel off one partof the film. Try not to touch the adhesive part of the patch. |
|
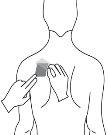
Step 3: Stick the transdermal patch to the area of skin you have chosen and remove the rest of the film. |
|
Step 4: Press the transdermal patch against your skin with the palm of your hand for 30 to 60 seconds. Make sure the entire patch is in contact with your skin, especially the edges. |
|
Step 5: Wash your hands after using the transdermal patch. Do not use any cleaning products. |
While wearing the transdermal patch
You can wear the transdermal patch for up to 4 days. If you have applied the transdermal patch correctly, the risk of it coming off is low. You can shower, bathe, or swim while wearing it. However, do not expose the transdermal patch to extreme heat (e.g., sauna, infrared lamps, electric blankets, or hot water bottles).
In the unlikely event that your transdermal patch falls off before you need to change it, do not use the same patch again. Apply a new one immediately (see "Changing the transdermal patch" below).
Changing the transdermal patch
- Remove the old patch carefully.
- Fold it in half with the adhesive side inward.
- Dispose of it carefully.
- Apply a new transdermal patch to a different area of skin (as described above). At least 1 week should pass before you can apply a new patch to the same area of skin.
Duration of treatment
Your doctor will indicate the duration of your treatment with buprenorphine. Do not stop treatment on your own, as the pain may return and you may feel unwell (see also "If you stop treatment with Buprenorphine Stada").
If you think the effect of buprenorphine is too strong or too weak, tell your doctor or pharmacist.
If you use more Buprenorphine Stada than you should
In case of overdose or accidental ingestion, consult your doctor or pharmacist immediately, or call the Toxicology Information Service, phone: 91 562 04 20, indicating the medication and the amount ingested. It is recommended to bring the packaging and the prospectus of the medication to the healthcare professional.
If this happens, there may be signs of buprenorphine overdose. An overdose can intensify the adverse effects of buprenorphine, such as drowsiness, nausea, and vomiting. You may have pinpoint pupils, and your breathing may become slow and weak. You could also suffer a cardiovascular collapse.
As soon as you realize you have used more buprenorphine transdermal patches than you should, remove the excess patches and consult your doctor or pharmacist immediately.
If you forget to use Buprenorphine Stada
If you forget an application, apply a new transdermal patch as soon as you remember.
This will make you change your routine, e.g., if you normally apply your transdermal patch on Mondays and Thursdays, but you forget and do not apply the new patch until Wednesday, from now on you will need to change your patches on Wednesdays and Saturdays. Note the new pair of days on the packaging calendar. If you change the patch too late, the pain may return. In this case, consult your doctor.
Never apply more than one transdermal patch to make up for the one you forgot!
If you stop treatment with Buprenorphine Stada
If you stop or finish treatment with buprenorphine too soon, the pain will return. If you want to stop treatment due to unpleasant side effects, consult your doctor. Your doctor will tell you what to do and if other medications can be administered.
Some people may have withdrawal effects after using potent painkillers for a long time and stopping them. The risk of having withdrawal effects after stopping buprenorphine is low. However, if you feel agitated, anxious, nervous, hyperactive, have sleep disorders, or digestive problems, consult your doctor.
If you have any other questions about using this medication, ask your doctor or pharmacist.
4. Possible side effects
Like all medications, this medication can cause side effects, although not everyone will experience them.
If you experience swelling of the hands, feet, knees, face, lips, mouth, or throat, which can cause difficulty swallowing or breathing, hives, fainting, yellowing of the skin and eyes (also called jaundice), remove the patch and consult your doctor or go to the nearest hospital immediately. These may be symptoms of a rare, severe allergic reaction.
The following side effects have been reported:
Very common(may affect more than 1 in 10 people):
- nausea (feeling of dizziness)
- erythema, pruritus
Common(may affect up to 1 in 10 people):
- dizziness, headache
- shortness of breath
- vomiting, constipation
- skin changes (rash, usually due to repeated use), increased sweating
- edema (swelling of the legs), fatigue
Uncommon(may affect up to 1 in 100 people):
- confusion, sleep disorders, restlessness
- different degrees of sedation (serenity), ranging from fatigue to confusion
- circulatory disorders (such as hypotension or rarely circulatory collapse)
- dry mouth
- rash
- urinary retention (less urine than normal), urination disorders
- weakness
Rare(may affect up to 1 in 1,000 people):
- loss of appetite
- hallucinations as well as illusions, anxiety, nightmares, decreased sexual desire
- difficulty concentrating, speech disorders, confusion, balance disorders, abnormal sensations in the skin (feeling of heat, tingling, or numbness)
- vision changes, blurred vision, eyelid swelling
- hot flashes
- breathing difficulties (respiratory depression)
- heartburn
- hives
- erection difficulties
- withdrawal symptoms (see below), administration site reactions
Very rare(may affect up to 1 in 10,000 people):
- severe allergic reactions (see below)
- dependence, mood changes
- muscle contraction, taste disorders
- pinpoint pupils
- ear pain
- abnormally rapid breathing, hiccups
- retching
- pustules, blisters
- chest pain
Frequency not known(frequency cannot be estimated from available data):
- contact dermatitis (skin rash with inflammation, which may include a burning sensation), skin discoloration.
If you notice any of the above side effects, consult your doctor as soon as possible.
In some cases, late local allergic reactions with marked signs of inflammation occur. In these cases, treatment with buprenorphine should be discontinued after consulting your doctor.
Some people may have withdrawal symptoms after using potent painkillers for a long time and stopping them. After treatment with buprenorphine, the risk of experiencing withdrawal symptoms is low. However, if you feel agitated, anxious, nervous, hyperactive, have sleep disorders, or digestive problems, consult your doctor.
Reporting side effects
If you experience any side effects, consult your doctor or pharmacist, even if they are possible side effects not listed in this prospectus. You can also report them directly through the Spanish Medicines Surveillance System for Human Use: https://www.notificaram.es. By reporting side effects, you can contribute to providing more information on the safety of this medication.
5. Storage of Buprenorphine Stada
Keep this medication out of sight and reach of children.
Do not use this medication after the expiration date shown on the packaging and on the pouch after CAD. The expiration date is the last day of the month indicated.
Store this medication in a safe and protected place, inaccessible to other people. This medication can cause serious harm and even be fatal if used accidentally or intentionally by people who have not been prescribed it.
This medication does not require special storage conditions.
After removing the patch, fold it in half with the adhesive surfaces inward and press firmly. Put the patch back in the pouch and dispose of it safely.
Medications should not be thrown down the drain or into the trash. Deposit the packaging and medications you no longer need at the SIGRE collection point in the pharmacy. Ask your pharmacist how to dispose of the packaging and medications you no longer need. This will help protect the environment.
6. Package contents and additional information
Composition of Buprenorphine Stada
- The active ingredient is buprenorphine.
Buprenorphine Stada 35 micrograms/hour: each transdermal patch of 25 cm2 contains 20 mg of buprenorphine and releases 35 micrograms of buprenorphine per hour.
Buprenorphine Stada 52.5 micrograms/hour: each transdermal patch of 37.5 cm2 contains 30 mg of buprenorphine and releases 52.5 micrograms of buprenorphine per hour.
Buprenorphine Stada 70 micrograms/hour: each transdermal patch of 50 cm2 contains 40 mg of buprenorphine and releases 70 micrograms of buprenorphine per hour.
- Other components are:
Adhesive matrix (containing buprenorphine): povidone K90, levulinic acid, oleyl oleate, poly(acrylic acid-co-butylacrylate-co-(2-ethylhexyl)acrylate-co-vinyl acetate) (5:15:75:5).
Adhesive matrix (without buprenorphine): poly((2-ethylhexyl)acrylate-co-glycidyl methacrylate-co-(2-hydroxyethyl)acrylate-co-vinyl acetate) (68:0.15:5:27).
Separator film between the adhesive matrices with and without buprenorphine: poly(ethylene terephthalate) film.
Supporting film: polyester.
Removable coating (on the front covering the adhesive matrix containing buprenorphine): siliconized polyethylene terephthalate film.
Blue printing ink.
Appearance of the product and package contents
Buprenorphine Stada 35 micrograms/hour: the transdermal patches are flesh-colored with rounded corners and are printed with "Buprenorphin" and "35 μg/h".
Buprenorphine Stada 52.5 micrograms/hour: the transdermal patches are flesh-colored with rounded corners and are printed with "Buprenorphin" and "52.5 μg/h".
Buprenorphine Stada 70 micrograms/hour: the transdermal patches are flesh-colored with rounded corners and are printed with "Buprenorphin" and "70 μg/h".
Each transdermal patch is individually sealed in a child-resistant pouch. The patches are available in packages containing 3, 4, 5, 6, 8, 10, 12, 16, 18, 20, or 24 transdermal patches.
Only some package sizes may be marketed.
Marketing authorization holder and manufacturer
Marketing authorization holder
Laboratorio STADA, S.L.
Frederic Mompou, 5
08960 Sant Just Desvern (Barcelona)
Spain
Manufacturer
Labtec GmbH
Heykenaukamp 10
21147 Hamburg
Germany
or
STADA Arzneimittel AG
Stadastraße 2-18
61118 Bad Vilbel
Germany
or
STADA Arzneimittel GmbH
Muthgasse 36
1190 Vienna
Austria
or
Laboratori Fundacio Dau
Calle Lletra C De La Zona Franca 12 – 14
Polígono Industrial De La Zona Franca De Barcelona
08040 Barcelona
Spain
This medication is authorized in the member states of the European Economic Area under the following names:
Germany: Buprenorphin AL 35 Mikrogamm/Stunde, Transdermales Pflaster
Buprenorphin AL 52,5 Mikrogamm/Stunde, Transdermales Pflaster
Buprenorphin AL 70 Mikrogamm/Stunde, Transdermales Pflaster
Austria: Buprenorphin STADA 35 Mikrogamm/h, Transdermales Pflaster
Buprenorphin STADA 52,5 Mikrogamm/h, Transdermales Pflaster
Buprenorphin STADA 70 Mikrogamm/h, Transdermales Pflaster
Denmark: Buprenorphin STADA
Spain: Buprenorfina STADA 35 microgramos/hora parche transdérmico 96 horas EFG
Buprenorfina Stada 52,5 microgramos/hora parche transdérmico 96 horas EFG
Buprenorfina Stada 70 microgramos/hora parche transdérmico 96 horas EFG
Netherlands: Buprenorfine CF 35 microgram/uur, pleister voor transdermaal gebruik
Buprenorfine CF 52,5 microgram/uur, pleister voor transdermaal gebruik
Buprenorfine CF 70 microgram/uur, pleister voor transdermaal gebruik
Portugal: Buprenorfina Ciclum
Date of the last revision of this prospectus:October 2024
Detailed and updated information on this medication is available on the website of the Spanish Agency for Medicines and Health Products (AEMPS) http://www.aemps.gob.es
- Country of registration
- Average pharmacy price43.04 EUR
- Active substance
- Prescription requiredYes
- Manufacturer
- This information is for reference only and does not constitute medical advice. Always consult a doctor before taking any medication. Oladoctor is not responsible for medical decisions based on this content.
- Alternatives to BUPRENORPHINE STADA 70 micrograms/hour transdermal patch 96 hoursDosage form: TRANSDERMAL PATCH, 35 micrograms/hourActive substance: buprenorphineManufacturer: Andromaco Pharma S.L.Prescription requiredDosage form: TRANSDERMAL PATCH, 52.5 micrograms/hourActive substance: buprenorphineManufacturer: Andromaco Pharma S.L.Prescription requiredDosage form: TRANSDERMAL PATCH, 70 micrograms/hourActive substance: buprenorphineManufacturer: Andromaco Pharma S.L.Prescription required
Online doctors for BUPRENORPHINE STADA 70 micrograms/hour transdermal patch 96 hours
Discuss questions about BUPRENORPHINE STADA 70 micrograms/hour transdermal patch 96 hours, including use, safety considerations and prescription review, subject to medical assessment and local regulations.
Frequently Asked Questions