How to use MYSOLINE 250 mg TABLETS
Translated with AI
This page provides general information and does not replace a doctor’s consultation. Always consult a doctor before taking any medication. Seek urgent medical care if symptoms are severe.
Show originalContents of the leaflet
Introduction
Package Leaflet: Information for the User
Mysoline 250 mg tablets
primidone
Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
- Keep this leaflet, you may need to read it again.
- If you have any further questions, ask your doctor or pharmacist.
- This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours.
- If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4.
Contents of the pack:
- What is Mysoline and what is it used for
- What you need to know before you take Mysoline
- How to take Mysoline
- Possible side effects
- Storing Mysoline
- Contents of the pack and other information
1. What is Mysoline and what is it used for
Mysoline tablets contain primidone as the active substance, which belongs to a group of medicines called anticonvulsants.
Mysoline is used to treat certain types of epilepsy, convulsions or seizures.
2. What you need to know before you take Mysoline
Do not take Mysoline
- If you are allergic (hypersensitive) to primidone, to a substance called phenobarbital, or to any of the other ingredients of this medicine (listed in section 6).
- If you have porphyria (a rare and inherited disorder of metabolism) or if anyone in your family has porphyria.
- If you are taking any of the following medicines at the same time:
- cholic acid (used to treat congenital bile acid synthesis deficiency),
- St. John's Wort (herb used to treat depression),
- isavuconazole or voriconazole (antifungal medicines),
- cobicistat, nelfinavir or rilpivirine (used to treat HIV infection),
- delamanid (used to treat tuberculosis),
- telaprevir, daclatasvir, dasabuvir, ombitasvir-paritaprevir, ledipasvir (used to treat hepatitis),
- lurasidone (used to treat schizophrenia),
- sofosbuvir (used to treat hepatitis C virus infection).
Warnings and precautions
This medicine is not effective in certain forms of epilepsy. Your doctor will assess the need for this treatment for you. Consult your doctor immediately if the frequency of your seizures increases or if different types appear.
Consult your doctor or pharmacist before starting to take Mysoline:
- if you have had respiratory, kidney or liver problems
- if you are pregnant or trying to become pregnant (see the information included later).
If you are going to the hospital, inform the healthcare staff that you are taking Mysoline.
Your doctor may prescribe you vitamin D supplements (in case of long-term treatment).
A small number of people treated with antiepileptic medicines such as primidone have had thoughts of harming themselves or committing suicide. If you have these thoughts at any time, contact your doctor immediately.
There have been reports of potentially life-threatening skin rashes (Stevens-Johnson syndrome, toxic epidermal necrolysis or DRESS syndrome) with the use of Mysoline, which initially appear as reddish spots similar to targets or circular patches often with blisters on the trunk.
- Other signs to look for include ulcers in the mouth, throat, nose, genitals and conjunctivitis (red and inflamed eyes).
- These potentially life-threatening skin rashes are often accompanied by symptoms similar to a cold. The rash may progress to generalized blisters or peeling of the skin.
- The greatest risk of severe skin reactions occurs within the first few weeks of treatment.
- If you have developed Stevens-Johnson syndrome, toxic epidermal necrolysis or DRESS syndrome with the use of Mysoline or any other medicine that contains phenobarbital, you should never take these medicines again.
If you experience a rash or these skin symptoms, stop using primidone and go to your doctor immediately and explain that you are taking this medicine.
Other medicines and Mysoline
Tell your doctor or pharmacist if you are using, have recently used or might use any other medicines.
This is important because some medicines can affect the way Mysoline works, or Mysoline can affect the way other medicines work.
In particular, tell your doctor if you are using any of the following:
- other medicines used to treat epilepsy or other types of seizures (such as phenytoin, felbamate, valproic acid, carbamazepine, perampanel, oxcarbazepine, stiripentol, tiagabine, zonisamide),
- anticoagulants to prevent blood clots (such as acenocoumarol, phenindione, warfarin),
- barbiturates or benzodiazepines (such as sleeping pills),
- medicines used to treat severe pain, cough or as a substitute for morphine addiction (such as methadone, oxycodone or fentanyl),
- antibiotics (such as metronidazole, doxycycline, telithromycin),
- medicines for asthma (such as theophylline),
- medicines that contain hormones (such as the oral contraceptive pill, estroprogestatives, progestatives, ulipristal),
- thyroid hormones,
- medicines used to treat mental health problems or depression (such as tricyclic antidepressants, clozapine, lamotrigine, mianserin, quetiapine, sertraline),
- medicines that contain steroids,
- medicines used to treat cancer (such as abiraterone, axitinib, eribulin, ifosfamide, bosutinib, crizotinib, dabrafenib, dasatinib, erlotinib, gefitinib, imatinib, lapatinib, nilotinib, pazopanib, ruxolitinib, sorafenib, sunitinib, vandetanib, regorafenib, vemurafenib, vismodegib, cabozantinib, ceritinib, ibrutinib, olaparib, ponatinib, cabazitaxel, docetaxel, irinotecan, procarbazine),
- bedaquiline (used to treat tuberculosis),
- quinine (used to treat malaria),
- medicines used to treat viral infections such as HIV or hepatitis C (such as boceprevir, dolutegravir, lopinavir, maraviroc, ritonavir, simeprevir),
- antifungal medicines (albendazole, itraconazole, posaconazole),
- anticoagulants (such as apixaban, dabigatran, rivaroxaban or ticagrelor),
- folates (vitamin B9),
- medicines used to reduce immunity (immunosuppressants, such as cyclosporin, tacrolimus, sirolimus, everolimus),
- deferasirox (iron chelator),
- ivacaftor (medicine used to treat cystic fibrosis),
- medicines used to treat heart disease, high blood pressure or to regulate heart rhythms (such as antiarrhythmics class IA, calcium antagonists, bosentan, digitoxin, dronedarone, ivabradine, macitentan, nimodipine, propafenone, ranolazine or beta blockers (metoprolol, propranolol)),
- antiparasitic agent (albendazole, praziquantel).
Taking Mysoline with food and drink
Alcohol may interfere with Mysoline. Drinking alcoholic beverages is not recommended during treatment.
Pregnancy, breastfeeding and fertility
If you are pregnant or breastfeeding, think you may be pregnant or are planning to have a baby, ask your doctor or pharmacist for advice before taking this medicine.
Women of childbearing age must use an effective contraceptive method during treatment. Mysoline may make the contraceptive pill less effective. Therefore, you should use another effective contraceptive method while taking Mysoline. For this, consult your doctor (see "Other medicines and Mysoline").
If you are a woman of childbearing age, you must use an effective contraceptive method during treatment with Mysoline and for two months after treatment. Mysoline may affect the functioning of hormonal contraceptives, such as the contraceptive pill, and make them less effective in preventing pregnancy. Talk to your doctor, who will study with you the most suitable form of contraception to use while taking Mysoline.
If you are a woman of childbearing age and plan to become pregnant, consult your doctor before stopping contraception and becoming pregnant, about the possibility of switching to other suitable treatments to avoid exposing the unborn baby to primidone (and therefore to its main metabolite phenobarbital).
If taken during pregnancy, primidone, which is largely metabolized to phenobarbital, may cause serious birth defects and affect the development of the child as it grows. Birth defects that have been reported in studies include cleft lip (a split in the upper lip) and cleft palate (a split in the roof of the mouth) and heart defects. Other congenital anomalies have also been reported, such as hypospadias (a malformation of the penis), a smaller than normal head size, and facial, nail and finger anomalies. If you take phenobarbital during pregnancy, you have a higher risk than other women of having a child with birth defects that require medical treatment. In the general population, the basic risk of major birth defects is 2-3%. This risk increases about 3 times in women taking phenobarbital.
Do not stop your treatment suddenly and contact your doctor immediately. Your doctor will consider stopping treatment or judging the potential benefit of continuing treatment in the absence of a less risky alternative for the fetus, in which case:
- During pregnancy: your doctor will adjust the dose to achieve the minimum effective dose for you and establish specialized prenatal monitoring that is appropriate for your specific case and the treatment you are following.
- Before delivery: you should take vitamin K to prevent bleeding that this medicine may cause during the first 24 hours of your baby's life.
- After delivery: an injection of vitamin K may also be prescribed for your baby at birth to prevent any bleeding.
You should not breastfeed if you are taking this medicine. Consult your doctor immediately if you are breastfeeding or if you want to breastfeed.
Babies born to mothers treated with phenobarbital during pregnancy may also be at risk of being smaller than expected.
There have been reports of developmental disorders (delays in development due to disorders in brain development) in children exposed to phenobarbital (primidone in Mysoline is mainly converted to phenobarbital) during pregnancy. Studies related to the risk of developmental disorders are contradictory.
Mysoline should not be used during pregnancy unless no other treatment is effective.
Talk to your doctor immediately if you are pregnant. Your doctor must study the possible effects of Mysoline tablets on the unborn baby, and the risks and benefits of treatment must be carefully considered. Do not stop treatment with primidone until you have consulted your doctor, as sudden interruption may increase the risk of developing seizures, which can have harmful effects on you and the unborn baby.
If you take Mysoline during the last trimester of pregnancy, appropriate follow-up should be carried out to detect potential disorders in the newborn, such as seizures, excessive crying, muscle weakness and sucking disorders.
Driving and using machines
Primidone may cause symptoms such as drowsiness, dizziness or vision changes, and reduce your reaction ability. These effects, as well as the disease itself, may make it difficult for you to drive vehicles or operate machines. Therefore, do not drive, operate machines, or engage in other activities that require special attention until your doctor assesses your response to this medicine.
3. How to take Mysoline
Always take Mysoline exactly as your doctor has told you.
If you are unsure, consult your doctor or pharmacist again.
Swallow the tablets whole with a little water. The tablet can be divided into equal doses.
The dose will be determined by your doctor and adjusted gradually on an individual basis.
Mysoline is usually taken twice a day. Try to take the tablets at the same time every day.
Initially, the dose may be as low as half a tablet. Your doctor will adjust it until your illness is controlled. The usual maintenance doses are as follows:
Age group | Number of tablets per day | Daily dose (milligrams) |
Adults and children over 9 years | 3 to 6 | 750 to 1,500 |
Children from 6 to 9 years | 3 to 4 | 750 to 1,000 |
Children from 2 to 5 years | 2 to 3 | 500 to 750 |
Children up to 2 years | 1 to 2 | 250 to 500 |
Elderly, debilitated patients and patients with kidney or liver disease:
May need lower doses. Please consult your doctor.
If you take more Mysoline than you should
If you take more than the normal dose, contact your doctor or go to the nearest hospital.
If you forget to take Mysoline
If you forget to take a dose, take it as soon as you remember. Do not take a double dose to make up for forgotten doses.
If you stop taking Mysoline
Do not stop taking Mysoline, even if you feel well, unless your doctor tells you to. You may have developed a dependence on Mysoline and therefore may suffer from withdrawal symptoms if you stop treatment too abruptly. To prevent this, treatment with Mysoline should be gradually reduced.
If you have any other questions about the use of this product, ask your doctor or pharmacist.
4. Possible side effects
Like all medicines, this medicine can cause side effects, although not everybody gets them.
Very rare(may affect up to 1 in 10,000 people)
- Potentially life-threatening skin rashes (Stevens-Johnson syndrome, toxic epidermal necrolysis) (see section 2) have been reported.
Frequency not known(cannot be estimated from the available data)
- Lack of energy (apathy), coordination disorders, visual disturbances, eye rolling.
- Nausea.
- Headache, dizziness, drowsiness.
- Vomiting.
- Allergic skin reaction.
- Exfoliative dermatitis (redness and peeling of the skin).
- Potentially fatal skin rashes (drug reaction with eosinophilia and systemic symptoms) (see section 2) have been reported.
- Itching (pruritus).
- Decrease in the number of some blood cells (red blood cells, white blood cells or platelets) or development of lymph nodes.
- Changes in mood or behavior, libido disorders.
- Pain in the joints or bones, Dupuytren's contracture (a thickening of the fibrous tissue in the palm of the hand that causes the retraction of one or more fingers).
- Systemic lupus erythematosus (a disease that causes inflammation of various parts of the body, including the skin, joints, lungs, kidneys, heart and liver).
- Elevated levels of liver enzymes (gamma GT, alkaline phosphatase).
- Suicidal thoughts
- Confusion
- Hallucinations
- Balance disorder
- Allergic reactions that may include fever, rash, increased number of some blood cells (eosinophils), increased liver enzymes.
- There have been reports of bone disorders including osteopenia and osteoporosis (thinning of the bone) and fractures. Consult your doctor or pharmacist if you are taking antiepileptic medicines for a long time, have a history of osteoporosis or take steroids.
- Osteomalacia (softening of the bones due to vitamin D deficiency).
- Decreased appetite, fatigue.
Reporting of side effects
If you experience any side effects, talk to your doctor or pharmacist, even if it is possible side effects not listed in this leaflet. You can also report them directly through the Spanish Pharmacovigilance System for Human Use Medicines: https://www.notificaram.es. By reporting side effects, you can help provide more information on the safety of this medicine.
5. Storing Mysoline
Keep this medicine out of the sight and reach of children.
Do not store above 25°C.
Do not use this medicine after the expiry date which is stated on the carton after EXP. The expiry date is the last day of the month shown.
Medicines should not be disposed of via wastewater or household waste. Place the packaging and any unused medicine in the SIGRE collection point at the pharmacy. If you are unsure, ask your pharmacist how to dispose of the packaging and any unused medicine. This will help protect the environment.
6. Packaging Content and Additional Information
Mysoline Composition
The active ingredient is primidone. Each tablet contains 250 mg of primidone.
The other components are calcium carmellose, gelatin, magnesium stearate, povidone, and stearic acid.
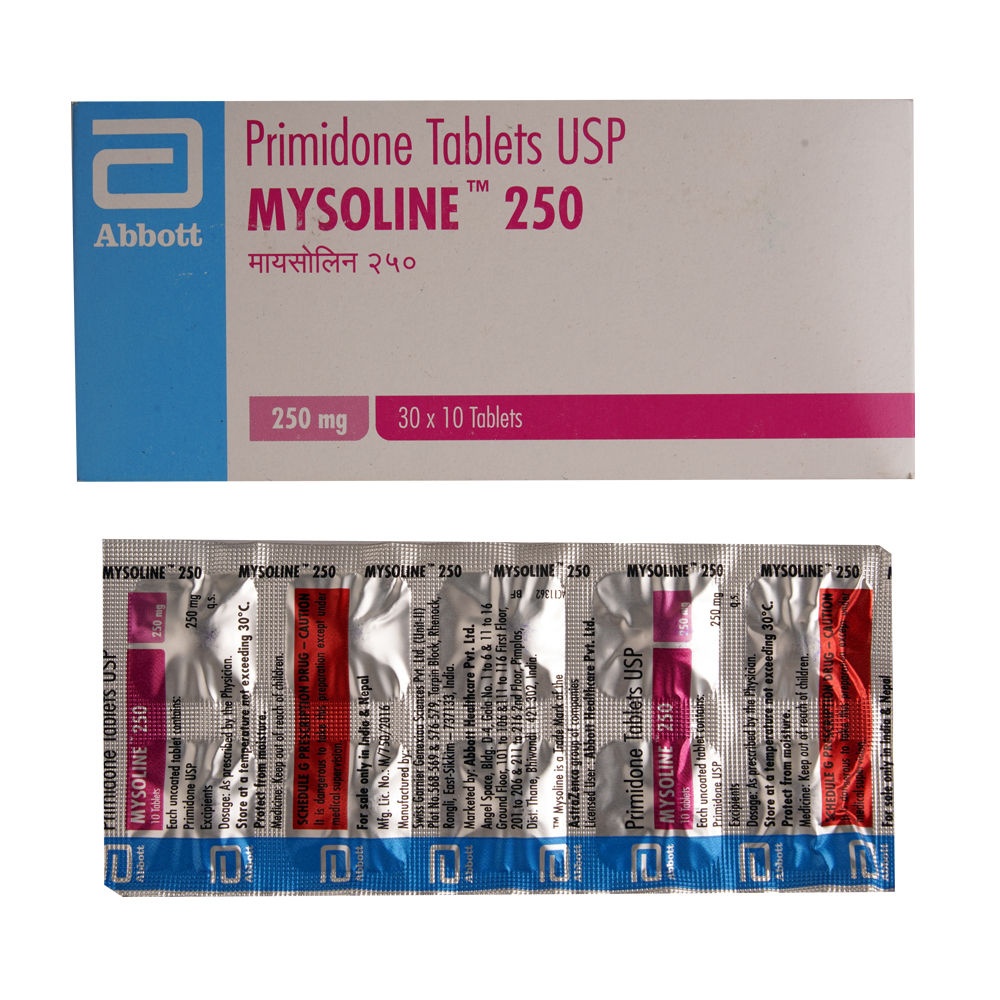
Product Appearance and Packaging Content
The tablets are round, white, and uncoated. One side of the tablet has the letter "M" printed on either side of a score line. The other side is flat.
Mysoline is available in packages of 100 tablets.
Marketing Authorization Holder and Manufacturer
Marketing Authorization Holder
Laboratoires SERB,
40 Avenue George V,
75008 Paris – FRANCE
Manufacturer
allphamed PHARBIL Arzneimittel GmbH
Hildebrandstrasse 10-12
37081 Göttingen - GERMANY
Local Representative
LABORATORIOS RUBIÓ, S.A.
Carrer Indústria 29 - Polígon Industrial Comte de Sert
08755 Castellbisbal, Barcelona – SPAIN
Date of the Last Revision of this Leaflet:07/2024
Detailed and updated information on this medication is available on the website of the Spanish Agency for Medicines and Health Products (AEMPS): http://www.aemps.es/
-
- Country of registration
- Dosage formTABLET, 250 mg Primidone
- ATC codeN03AA03
- Average pharmacy price12.49 EUR
- Active substance
- Prescription requiredYes
- Manufacturer
- This information is for reference only and does not constitute medical advice. Always consult a doctor before taking any medication. Oladoctor is not responsible for medical decisions based on this content.
- Alternatives to MYSOLINE 250 mg TABLETSDosage form: TABLET, 100 mg phenobarbitalActive substance: phenobarbitalManufacturer: Kern Pharma S.L.Prescription requiredDosage form: INJECTABLE, 200 mg phenobarbitalActive substance: phenobarbitalManufacturer: Kern Pharma S.L.Prescription requiredDosage form: TABLET, 15 mg phenobarbitalActive substance: phenobarbitalManufacturer: Kern Pharma S.L.Prescription required
Online doctors for MYSOLINE 250 mg TABLETS
Discuss questions about MYSOLINE 250 mg TABLETS, including use, safety considerations and prescription review, subject to medical assessment and local regulations.
Get MYSOLINE 250 mg TABLETS Prescription Online
Fill in a 2-min form
Tell us your symptoms, history, and what medicine you're requesting.
Pick a doctor or let us assign
Choose a specialist or we'll match you with the next available doctor.
Doctor reviews your case
Usually within 30 minutes. They may ask follow-up questions via chat.
Collect from any pharmacy
Electronic prescription sent to your email — valid across Spain.
Frequently Asked Questions
MYSOLINE 250 mg TABLETS requires a prescription in Spain. You can check with a doctor online whether this medicine may be appropriate for your situation.
The active ingredient in MYSOLINE 250 mg TABLETS is primidone. This information helps identify medicines with the same composition but different brand names.
The average pharmacy price for MYSOLINE 250 mg TABLETS is around 12.49 EUR. Prices may vary depending on the manufacturer and dosage form.
MYSOLINE 250 mg TABLETS is manufactured by Serb. Pharmacy brands and packaging may differ depending on the distributor.
Doctors such as Family doctors, Psychiatrists, Dermatologists, Cardiologists, Endocrinologists, Gastroenterologists, Pulmonologists, Nephrologists, Rheumatologists, Hematologists, Infectious disease physicians, Allergists, Geriatricians, Paediatricians, Oncologists may assess whether MYSOLINE 250 mg TABLETS is appropriate, depending on your situation and local regulations. You can book an online consultation to discuss your symptoms and possible next steps.
Spain has a well-developed healthcare infrastructure across major cities such as Madrid, Barcelona, Valencia, and Seville. Pharmacies are widely available and operate under strict regulations, ensuring access to prescribed medications.
You can buy MYSOLINE 250 mg TABLETS in Madrid, Barcelona, Seville, or Valencia at any local pharmacy with a valid prescription.
To obtain a prescription, you can use Oladoctor:
Other medicines with the same active substance (primidone) include LUMINAL 100 mg TABLETS, LUMINAL 200 mg/mL Injectable Solution, LUMINALETAS 15 mg TABLETS. These may have different brand names or formulations but contain the same therapeutic ingredient. Always consult a doctor before switching or starting a new medicine.