How to use ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen
Translated with AI
This page provides general information and does not replace a doctor’s consultation. Always consult a doctor before taking any medication. Seek urgent medical care if symptoms are severe.
Show originalContents of the leaflet
Introduction
Package Leaflet: Information for the User
Actrapid InnoLet 100IU/ml (International Units/ml) solution for injection in a pre-filled pen
human insulin
Read all of this leaflet carefully before you start using this medicine because it contains important information for you.
- Keep this leaflet, you may need to read it again.
- If you have any further questions, ask your doctor, pharmacist, or nurse.
- This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours.
- If you get any side effects, talk to your doctor, pharmacist, or nurse. This includes any possible side effects not listed in this leaflet. See section 4.
Contents of the pack
- What is Actrapid and what is it used for
- What you need to know before you use Actrapid
- How to use Actrapid
- Possible side effects
- Storing Actrapid
- Contents of the pack and other information
1. What is Actrapid and what is it used for
Actrapid is a fast-acting human insulin.
Actrapid is used to reduce high blood sugar levels in patients with diabetes mellitus (diabetes). Diabetes is a disease where your body does not produce enough insulin to control your blood sugar levels. Treatment with Actrapid helps to prevent complications of diabetes.
Actrapid starts to lower your blood sugar level about 30 minutes after injection and the effect lasts for approximately 8 hours. Actrapid is usually given in combination with intermediate or long-acting insulin preparations
2. What you need to know before you use Actrapid
Do not use Actrapid
?If you are allergic to human insulin or any of the other ingredients of this medicine, see section 6.
?If you suspect you are starting to get hypoglycaemia (low blood sugar), see Summary of serious and frequent side effects in section 4.
? In insulin infusion pumps.
? If your InnoLet has been dropped, damaged, or broken.
?If it has not been stored correctly or has been frozen, see section 5.
? If the insulin does not look like water and is not clear.
If any of these apply, do not use Actrapid. Talk to your doctor, pharmacist, or nurse.
Before using Actrapid
? Check the label to make sure it is the right type of insulin.
? Always use a new needle for each injection to avoid contamination.
? Needles and Actrapid InnoLet must not be shared.
? Actrapid InnoLet is only intended for injection under the skin. Talk to your doctor if you need to inject the insulin by another method.
Warnings and precautions
Some changes and activities can affect your insulin needs. Talk to your doctor:
?If you have kidney, liver, adrenal, pituitary, or thyroid problems.
?If you do more physical exercise than usual or want to change your usual diet, as this may affect your blood sugar level.
?If you are ill, you must keep using insulin and talk to your doctor.
?If you are going abroad, travelling across time zones may affect your insulin requirements and the timing of your injections.
Changes at the injection site
You should rotate the injection site to help avoid changes in the fatty tissue under the skin, such as lumps, thickening, or pitting. Insulin may not work well if you inject into a lumpy, thickened, or pitted area (see section 3). Tell your doctor if you notice any changes at the injection site. Tell your doctor if you are currently injecting in these affected areas before starting to inject in a different area. Your doctor may tell you to check your blood sugar levels more closely and adjust your insulin dose or other anti-diabetic medications.
Other medicines and Actrapid
Tell your doctor, pharmacist, or nurse if you are taking, have recently taken, or might take any other medicines.
Some medicines affect your blood sugar level, and this may mean you need to adjust your insulin dose. The following medicines are the most common ones that may affect your insulin treatment.
Your blood sugar level may fall (hypoglycaemia) if you take:
- Other medicines for the treatment of diabetes
- Monoamine oxidase inhibitors (MAOIs) (used to treat depression)
- Beta-blockers (used to treat high blood pressure)
- Angiotensin-converting enzyme (ACE) inhibitors (used to treat certain heart conditions or high blood pressure)
- Salicylates (used to relieve pain and lower fever)
- Anabolic steroids (such as testosterone)
- Sulphonamides (used to treat infections)
Your blood sugar level may rise (hyperglycaemia) if you take:
- Oral contraceptives (birth control pills)
- Thiazides (used to treat high blood pressure or excessive fluid retention)
- Corticosteroids (such as cortisone, used to treat inflammation)
- Thyroid hormone (used to treat thyroid disorders)
- Sympathomimetics (such as adrenaline, salbutamol, or terbutaline, used to treat asthma)
- Growth hormone (used to stimulate bone and somatic growth and has significant influence on the body's metabolic processes)
- Danazol (a medicine that affects ovulation)
Octreotide and lanreotide (used to treat acromegaly, a rare hormonal disorder that usually occurs in middle-aged adults, caused by excess growth hormone production in the pituitary gland) may increase or decrease your blood sugar level.
Beta-blockers (used to treat high blood pressure) may weaken or completely suppress the first warning symptoms that help you recognise a low blood sugar level.
Pioglitazone (tablets used to treat type 2 diabetes)
Some patients with type 2 diabetes of long duration and heart disease or previous stroke who were treated with pioglitazone and insulin developed heart failure. Tell your doctor as soon as possible if you have signs of heart failure such as unusual shortness of breath, rapid weight gain, or localised swelling (oedema).
If you have taken any of the medicines listed above, tell your doctor, pharmacist, or nurse.
Using Actrapid with alcohol
? If you drink alcohol, your insulin needs may change, as your blood sugar level may increase or decrease. You are advised to keep a close watch on your blood sugar levels.
Pregnancy and breast-feeding
? If you are pregnant, think you may be pregnant, or are planning to have a baby, ask your doctor for advice before taking this medicine. Actrapid can be used during pregnancy. You may need to adjust your insulin dose during pregnancy and after delivery. Keeping a close watch on your diabetes, especially to prevent hypoglycaemia, is important for the health of your baby.
? There are no restrictions on the use of Actrapid during breast-feeding.
Ask your doctor, pharmacist, or nurse for advice before taking this medicine during pregnancy or breast-feeding.
Driving and using machines
?Ask your doctor whether you can drive or use machines:
- If you often get hypoglycaemia.
- If you have difficulty recognising the warning signs of hypoglycaemia.
If your blood sugar is high or low, it may affect your concentration and reaction ability, and therefore also your ability to drive or use machines. You may put yourself or others at risk.
Actrapid contains sodium
Actrapid contains less than 1 mmol of sodium (23 mg) per dose, which is essentially “sodium-free”.
3. How to use Actrapid
Dose and when to use the insulin
Follow exactly the instructions for administration of this medicine and the dose given by your doctor. If you are not sure, talk to your doctor, pharmacist, or nurse.
Eat a meal or snack containing carbohydrates within 30 minutes of the injection to avoid a drop in blood sugar level.
Do not change your insulin unless your doctor tells you to. If your doctor switches you from one type or brand of insulin to another, you may need to adjust your dose.
Use in children and adolescents
Actrapid can be used in children and adolescents.
Use in special patient groups
If you have kidney or liver problems or if you are over 65 years old, you should check your blood sugar level more often and talk to your doctor about possible changes in your insulin dose.
How and where to inject the insulin
Actrapid is administered by injection under the skin (subcutaneous injection). It should never be injected directly into a vein (intravenous injection) or muscle (intramuscular injection). Actrapid InnoLet is only intended for injection under the skin. Talk to your doctor if you need to inject the insulin by another method.
With each injection, change the injection site within the area of skin you use. This may reduce the risk of developing lumps or hollows under the skin, see section 4. The best areas for injection are the front of your waist (abdomen), the buttocks, the front of your thighs, or the upper arm. The effect of the insulin will be faster if you inject into the abdomen. You should measure your blood sugar level regularly.
How to handle Actrapid InnoLet
Actrapid InnoLet is a pre-filled disposable pen containing human insulin.
Read carefully the Instructions for using Actrapid InnoLet included in this package leaflet. You must use the pen as described in the Instructions for using Actrapid InnoLet.
Always make sure you use the correct pen before injecting.
If you use more insulin than you should
If you use too much insulin, your blood sugar level may become too low (hypoglycaemia). See Summary of serious and frequent side effects in section 4.
If you forget to use your insulin
If you forget to use your insulin, your blood sugar level may become too high (hyperglycaemia). See Effects of diabetes in section 4.
If you stop using insulin
Do not stop using your insulin without talking to your doctor first. If you stop using your insulin, your blood sugar level may become very high (severe hyperglycaemia) and you may develop ketoacidosis. See Effects of diabetes in section 4.
If you have any further questions on the use of this medicine, ask your doctor, pharmacist, or nurse.
4. Possible Adverse Effects
Like all medicines, this medicine can cause adverse effects, although not all people suffer from them.
Summary of Serious and Very Common Adverse Effects
Decrease in Blood Sugar Level (Hypoglycemia)is a very common adverse effect. It can affect more than 1 in 10 people.
Blood sugar levels can drop if:
- Too much insulin is injected.
- Very little food is eaten or a meal is skipped.
- More physical exercise than usual is done.
- Alcohol is consumed; see Use of Actrapid with alcohol in section 2.
Signs of a drop in blood sugar level: cold sweat, cold and pale skin, headache, rapid heartbeat, feeling of discomfort, excessive appetite, temporary visual disturbances, drowsiness, unusual fatigue and weakness, nervousness or tremors, anxiety, confusion, and difficulty concentrating.
A severe drop in blood sugar level can lead to loss of consciousness. If the low blood sugar level persists and is not treated, it can cause brain damage (transient or permanent) and even death. You can regain consciousness more quickly if someone who knows how to do it administers a glucagon injection to you. If you are given glucagon, you should also take glucose or a sugary product as soon as you regain consciousness. If you do not respond to glucagon treatment, you must go to the hospital immediately.
What to do if you suffer a drop in blood sugar level:
? If you suffer a drop in blood sugar level, ingest glucose tablets or another product with high sugar content (e.g., candies, cookies, fruit juice). Measure your blood sugar level if possible, and rest. Always carry glucose tablets or products with high sugar content with you, just in case.
? When the symptoms of low blood sugar have disappeared or when your blood sugar level has stabilized, continue with the insulin treatment as usual.
? If your blood sugar level is so low that you faint, if you have needed a glucagon injection, or if you have suffered many episodes of low blood sugar, talk to your doctor. You may need to adjust the dose or frequency of insulin administration, your eating habits, or exercise.
Inform relevant people that you have diabetes and what the consequences may be, such as the risk of fainting (losing consciousness) due to low blood sugar. Let them know that if you faint, they should turn you onto your side and seek immediate medical help. They should not give you food or drinks, as you may choke.
Severe Allergic Reactionto Actrapid or one of its components (called a systemic allergic reaction) is a very rare but potentially life-threatening adverse effect. It can affect up to 1 in 10,000 people.
Consult your doctor immediately:
- If allergy symptoms spread to other parts of the body.
- If you suddenly feel unwell and have sweats, feeling of discomfort (nausea), difficulty breathing, rapid heartbeat, and a feeling of impending loss of consciousness.
? If you notice any of these symptoms, seek medical help immediately.
Changes in the Skin at the Injection Site: If insulin is injected in the same place, the fatty tissue can shrink (lipoatrophy) or become thicker (lipohypertrophy) (can affect up to 1 in 100 people). Lumps under the skin can also occur due to the accumulation of a protein called amyloid (cutaneous amyloidosis; the frequency of this is unknown). Insulin may not work as well if it is injected into a lumpy, shrunken, or thickened area. Change the injection site to help avoid these skin changes.
List of Other Adverse Effects
Uncommon Adverse Effects
Can affect up to 1 in 100 people.
Allergy Symptoms:local allergic reactions (pain, redness, rash, inflammation, bruising, swelling, and itching) can occur at the injection site. They usually disappear within a few weeks of starting insulin use. If they do not disappear or spread throughout the body, talk to your doctor immediately. Also, see the severe allergic reactions mentioned earlier.
Vision Problems:when starting insulin treatment, it can affect your vision, but usually only temporarily.
Joint Inflammation:when starting insulin treatment, fluid accumulation can cause inflammation of the ankles and other joints. This effect usually disappears quickly. If it does not, talk to your doctor.
Painful Neuropathy(nerve damage-related pain): if your blood sugar level improves very quickly, you may experience pain related to the nerves. This is known as acute painful neuropathy and is usually transient.
Very Rare Adverse Effects
Can affect up to 1 in 10,000 people.
Diabetic Retinopathy(eye disease related to diabetes that can lead to vision loss): if you have diabetic retinopathy and your blood sugar level improves very quickly, retinopathy can worsen. In this case, you should consult your doctor.
Reporting Adverse Effects
If you experience any type of adverse effect, consult your doctor, pharmacist, or nurse, even if it is a possible adverse effect not listed in this leaflet. You can also report them directly through the Spanish Medicines Monitoring System for Human Use: www.notificaRAM.es. By reporting adverse effects, you can contribute to providing more information on the safety of this medicine.
Effects Derived from Diabetes
High Blood Sugar Level (Hyperglycemia)
You may experience high blood sugar levels if:
- Not enough insulin is injected.
- You forget to inject insulin or stop using it.
- You repeatedly inject less insulin than you need.
- You have an infection and/or fever.
- You eat more than usual.
- You do less physical exercise than usual.
Warning signs of high blood sugar levels:
The warning signs appear gradually and include excessive urination, thirst, loss of appetite, feeling of discomfort (nausea and vomiting), drowsiness or fatigue, dry and reddened skin, dry mouth, and fruity breath odor (acetone).
What to do if you suffer from high blood sugar levels:
? If you experience any of the above symptoms: check your blood sugar and ketone levels in your urine if possible, and then seek medical help immediately.
? They can be symptoms of a very serious condition called diabetic ketoacidosis (acid buildup in the blood due to the body breaking down fat instead of sugar). If left untreated, it could lead to a diabetic coma and even death.
5. Storage of Actrapid
Keep this medicine out of the sight and reach of children.
Do not use this medicine after the expiration date stated on the label and packaging of the InnoLet after CAD. The expiration date is the last day of the month indicated.
Before Opening:store in a refrigerator (between 2°C and 8°C). Keep away from the cooling element. Do not freeze.
During Use or as a Spare:do not refrigerate or freeze. It can be carried and stored at room temperature (below 30°C) for up to 6 weeks.
Always keep the pen cap on your InnoLet when not in use to protect it from light.
Discard the needle after each injection.
Medicines should not be disposed of via wastewater or household waste. Ask your pharmacist how to dispose of the packaging and medicines you no longer need. This will help protect the environment.
6. Package Contents and Additional Information
Composition of Actrapid
- The active ingredient is human insulin. Each ml contains 100 IU of human insulin. Each pre-filled pen contains 300 IU of human insulin in 3 ml of injectable solution.
- The other ingredients are zinc chloride, glycerol, metacresol, sodium hydroxide, hydrochloric acid, and water for injectable preparations.
Appearance of the Product and Package Contents
Actrapid is presented as an injectable solution.
Package sizes of 1, 5, and 10 pre-filled pens of 3 ml. Not all package sizes may be marketed.
The solution is transparent and colorless.
Marketing Authorization Holder and Manufacturer
Novo Nordisk A/S, Novo Allé, DK-2880 Bagsværd, Denmark
Date of the Last Revision of this Leaflet:
Other Sources of Information
Detailed information on this medicine is available on the European Medicines Agency website: http://www.ema.europa.eu.
Instructions for Use are Included on the Backof the Leaflet.
Instructions for Using Actrapid Injectable Solution in InnoLet.
Read the Instructions Carefully Before Using Your InnoLet.If you do not follow the instructions carefully, you may administer too little or too much insulin, which could result in a blood sugar level that is too high or too low.
InnoLet is a simple and compact pre-filled pen capable of administering doses from 1 to 50 units, in increments of 1 unit. InnoLet is designed to be used with disposable NovoFine or NovoTwist needles up to 8 mm in length. As a precaution, always carry a spare insulin delivery device with you in case your InnoLet is lost or damaged.
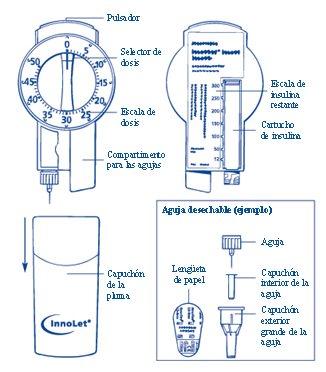
First Steps
Check the Name and Color Labelof your InnoLet to ensure it contains the correct type of insulin. This is especially important if you use more than one type of insulin. If you use the wrong type of insulin, your blood sugar level can become too high or too low. Remove the pen cap.
Attaching the Needle
- Always use a new needle for each injection. This reduces the risk of contamination, infection, insulin loss, needle blockage, and inaccurate dosing.
- Be careful not to bend or damage the needle before use.
- Remove the paper tab from a new disposable needle.
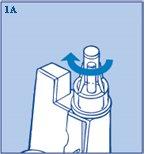
- Screw the needle straight and firmly onto the InnoLet (figure 1A).
- Remove the large outer needle cap and the inner needle cap. You can store the large outer needle cap in the compartment.
Never attempt to put the inner needle cap back on. You could stick yourself with the needle.
Preparing to Expel Air Before Each Injection
During use, small amounts of air may remain in the needle and insulin cartridge.
To avoid injecting air and ensure accurate dosing:
- Set 2 units by turning the dose selector clockwise.
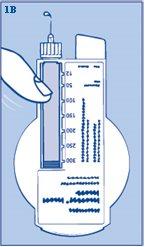
- Hold your InnoLet with the needle pointing upwards and gently tap the cartridge with your finger several times (figure 1B) to make any air bubbles rise to the top of the cartridge.
- With the needle still pointing upwards, press the push button and the dose selector will return to 0.
- Always make sure a drop appears at the needle tip before injecting (figure 1B). This ensures that the insulin is flowing. If this does not happen, change the needle and repeat the procedure up to 6 times.
If a drop of insulin still does not appear, the device is defective and should not be used.
- If a drop does not appear, no insulin will be injected, even if the dose selector moves. This may indicate that the needle is blocked or damaged.
- Always check your InnoLet before injecting. If you do not check your InnoLet, you may receive an insufficient or non-existent amount of insulin. This could result in a blood sugar level that is too high.
Dose Selection
- Always ensure the push button is fully depressed and the dose selector is set to 0.
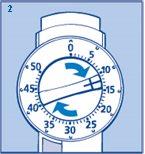
- Set the required number of units by turning the dose selector clockwise (figure 2).
- You will hear a click for each unit dialed. The dose can be corrected by turning the dose selector in both directions. Ensure you do not turn the dose selector or correct the dose once the needle is under your skin. This could result in inaccurate dosing, causing your blood sugar level to become too high or too low.
Always use the dose selector and dose marker to see how many units you have selected before injecting the insulin. Do not count the clicks of the pen. If you select an incorrect dose and inject it, your blood sugar level can become too high or too low. Do not use the remaining insulin scale, as it only shows the approximate amount of insulin left in the pen.
You cannot select a dose greater than the number of units remaining in the cartridge.
Injecting the Insulin
- Insert the needle under the skin. Use the injection technique recommended by your doctor.
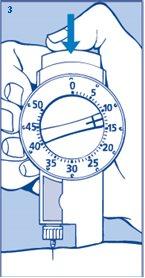
- Administer the dose by pressing the push button fully (figure 3). You will hear clicks as the dose selector returns to 0.
- After the injection, keep the needle under the skin for at least 6 seconds to ensure the full dose is administered.
- Make sure you do not block the dose selector while injecting, as the dose selector must return to 0 as you press the push button. Always ensure the dose selector returns to 0 after the injection. If the dose selector stops before reaching 0, the full dose has not been administered, which could result in a blood sugar level that is too high.
- Discard the needle after each injection.
Removing the Needle
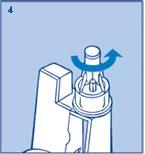
- Put the large outer needle cap back on and unscrew the needle (figure 4). Dispose of it carefully.
- Put the pen cap back on your InnoLet to protect the insulin from light.
Always use a new needle for each injection.
Always remove and discard the needle after each injection and store your InnoLet without the needle attached. This reduces the risk of contamination, infection, insulin loss, needle blockage, and inaccurate dosing.
Other Important Information
People caring for these patients should be very careful when handling used needles to reduce the risk of accidental needlestick injuries and infections.
Discard your used InnoLet carefully without leaving the needle attached.
Never share the pen or needles with others. This could lead to infections.
Never share the pen with others. Your medicine could be harmful to their health.
Always keep your InnoLet and needles out of sight and reach of others, especially children.
Care of the Pen
InnoLet is designed to function with precision and safety. It should be handled with care. If it is dropped, damaged, or knocked, there is a risk that insulin may leak out. This could cause inaccurate dosing, resulting in a blood sugar level that is too high or too low.
You can clean your InnoLet with a cotton swab dipped in alcohol. Do not submerge, wash, or lubricate it. This can damage the mechanism and cause inaccurate dosing, resulting in a blood sugar level that is too high or too low.
Do not refill your InnoLet. Once empty, it should be discarded.
-
- Country of registration
- Dosage formINJECTABLE, 100 U/ml
- ATC codeA10AB01
- Active substance
- Prescription requiredYes
- Manufacturer
- This information is for reference only and does not constitute medical advice. Always consult a doctor before taking any medication. Oladoctor is not responsible for medical decisions based on this content.
- Alternatives to ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled penDosage form: INJECTABLE, 100 U/mlActive substance: insulin (human)Manufacturer: Novo Nordisk A/SPrescription requiredDosage form: INJECTABLE, 100 IU/mLActive substance: insulin (human)Manufacturer: Lilly S.A.Prescription requiredDosage form: INJECTABLE, 100 IU/mlActive substance: insulin (human)Manufacturer: Sanofi-Aventis Deutschland GmbhPrescription required
Online doctors for ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen
Discuss questions about ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen, including use, safety considerations and prescription review, subject to medical assessment and local regulations.
Get ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen Prescription Online
Fill in a 2-min form
Tell us your symptoms, history, and what medicine you're requesting.
Pick a doctor or let us assign
Choose a specialist or we'll match you with the next available doctor.
Doctor reviews your case
Usually within 30 minutes. They may ask follow-up questions via chat.
Collect from any pharmacy
Electronic prescription sent to your email — valid across Spain.
Frequently Asked Questions
ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen requires a prescription in Spain. You can check with a doctor online whether this medicine may be appropriate for your situation.
The active ingredient in ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen is insulin (human). This information helps identify medicines with the same composition but different brand names.
ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen is manufactured by Novo Nordisk A/S. Pharmacy brands and packaging may differ depending on the distributor.
Doctors such as Family doctors, Psychiatrists, Dermatologists, Cardiologists, Endocrinologists, Gastroenterologists, Pulmonologists, Nephrologists, Rheumatologists, Hematologists, Infectious disease physicians, Allergists, Geriatricians, Paediatricians, Oncologists may assess whether ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen is appropriate, depending on your situation and local regulations. You can book an online consultation to discuss your symptoms and possible next steps.
Spain has a well-developed healthcare infrastructure across major cities such as Madrid, Barcelona, Valencia, and Seville. Pharmacies are widely available and operate under strict regulations, ensuring access to prescribed medications.
You can buy ACTRAPID INNOLET 100 IU/mL Injectable solution in a prefilled pen in Madrid, Barcelona, Seville, or Valencia at any local pharmacy with a valid prescription.
To obtain a prescription, you can use Oladoctor:
Other medicines with the same active substance (insulin (human)) include ACTRAPID 100 IU/mL INJECTABLE SOLUTION IN A VIAL, HUMULINA REGULAR 100 IU/ML INJECTABLE SOLUTION IN VIAL, INSUMAN INFUSAT 100 IU/ml INJECTABLE SOLUTION IN A CARTRIDGE. These may have different brand names or formulations but contain the same therapeutic ingredient. Always consult a doctor before switching or starting a new medicine.